(VOVWORLD) - Type 2 diabetes is one of the most common chronic conditions worldwide, yet many people may live with it for years without noticing clear symptoms. In this episode of Doctor at Home, we speak with Dr. Dinh Trung Hoa, a specialist in internal medicine and endocrinology who cares for patients with diabetes, thyroid diseases, and other metabolic disorders. Drawing on his daily experience working with patients and their families, Dr. Hoa explains what happens in the body when Type 2 diabetes develops, the warning signs people should watch for, and why early screening is important. He also highlights the important role caregivers play in supporting patients at home.
Reporter: Doctor Hoa, thank you for joining us today. First, could you explain what Type 2 diabetes is and why this condition can remain “silent” in the early stages?
Dr. Trung Hoa: Type 2 diabetes is a condition where the sugar level in the blood becomes too high over time. Normally, after we eat, sugar from food enters the blood. The body uses a hormone called insulin to move that sugar into the cells, where it becomes energy. In Type 2 diabetes, the body’s cells become less responsive to insulin, so sugar does not move into the cells as easily. At the same time, the pancreas, the organ that makes insulin, may gradually produce less insulin as it gets “tired.”
Early on, the body tries to compensate by making more insulin, so blood sugar rises slowly. That’s why many people feel normal for years. They may not have pain, fever, or strong symptoms. But even if you feel fine, high sugar can quietly damage blood vessels and nerves. This is why screening is important, especially for people with risk factors like overweight, family history, high blood pressure, or older age.
Reporter: What warning signs should people watch for, and why do some patients have no obvious symptoms until complications appear?
Dr. Trung Hoa: Common warning signs include feeling very thirsty, urinating more often (especially at night), dry mouth, tiredness, blurry vision, slow healing of wounds, frequent skin infections, frequent urinary infections, and sometimes unexpected weight loss. Some people also feel tingling or numbness in the feet.
However, many patients have no clear symptoms because the sugar level increases gradually. The body adapts, and people may think tiredness is just work stress or aging. Also, some symptoms are non-specific, meaning they can be caused by many problems. In some cases, the first time diabetes is discovered is when complications appear, like heart disease, kidney problems, eye disease, or a serious infection. That is why it is safer to check blood glucose early rather than waiting for symptoms.
Reporter: Many people also hear about prediabetes. What exactly does this mean, and can it be reversed?
Dr. Trung Hoa: Prediabetes means blood sugar is higher than normal, but not high enough to be called diabetes. I often describe it as a “yellow light” warning. It is serious because it increases the chance of developing diabetes and also increases the risk of heart and blood vessel disease. The encouraging part is that prediabetes can often be improved, and in many people, it can return to a normal range. Weight loss helps, even a small amount. Regular physical activity helps the body use sugar better. A healthier eating pattern, less sugary drinks, fewer refined carbohydrates like sweets and white flour foods, and more vegetables, protein, and whole foods, can make a real difference. Good sleep and stress control also matter because poor sleep and chronic stress can worsen blood sugar control. The earlier we act, the better the results.
Reporter: There are many misconceptions about diabetes. What are the most common misconceptions that you would like to clarify?
Dr Trung Hoa: One misconception is, “If I don’t eat sugar, I won’t get diabetes.” In reality, diabetes is influenced by many factors, overall diet, body weight, physical activity, sleep, stress, and genetics. Another misconception is, “I feel okay, so my diabetes is not serious.” Diabetes can be silent while still causing damage.
Some people believe, “Herbal products alone can replace medical treatment.” Some supplements may be harmless but relying on them instead of proven treatment can be dangerous. Another common misunderstanding is, “If I start using insulin, it means I failed.” Not at all. Insulin is simply one tool. Sometimes it is needed because the body no longer produces enough insulin. Using insulin can protect organs and prevent complications. Finally, some think, “Medicine is enough, lifestyle doesn’t matter.” In fact, medicine works best when combined with good daily habits.
Dr. Dinh Trung Hoa graduated with distinction from the Russian National Research Medical University and joined the National Hospital of Endocrinology in Vietnam in 2020.
He is currently a PhD candidate at Hanoi Medical University, specializing in endocrinology. His professional activities span clinical care, research, and academic writing, with broader interests in endocrinology, internal medicine, and gerontology.
His research focuses particularly on diabetes and age-related conditions, reflecting a strong commitment to improving the management and long-term outcomes of older adults with chronic endocrine and metabolic disorders. By integrating clinical experience with academic training, he is building a career as a dedicated physician-scientist in endocrine medicine.
Reporter: That was some information about Dr. Dinh Trung Hoa, who is talking with us today. Doctor Hoa! If diabetes is not well controlled, what kinds of health complications can develop?
Dr Trung Hoa: Uncontrolled diabetes can affect many organs. High sugar damages small blood vessels and nerves, which can lead to eye disease and vision loss, kidney damage that may progress to kidney failure, and nerve damage that causes numbness or burning pain, often starting in the feet. When the feet lose sensation, small wounds can be missed and become serious infections. Diabetes also increases the risk of heart attack and stroke. It can weaken the immune system, so infections happen more easily and wounds heal more slowly. Over time, people may also develop sexual health problems and higher risk of depression due to chronic illness. The key message for caregivers is that these complications are not inevitable. With regular monitoring, good blood sugar control, and follow-up care, the risk can be greatly reduced.
Reporter: For people living with diabetes, how can they manage the condition at home?
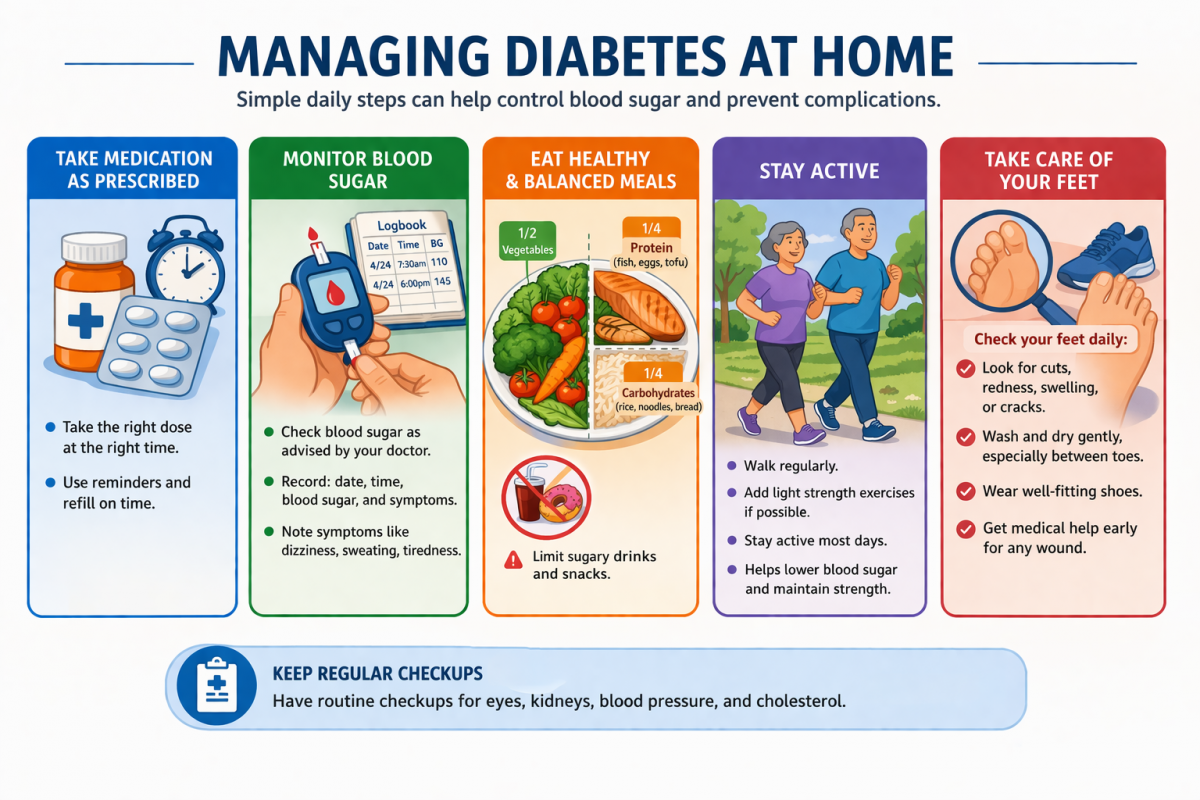
Dr Trung Hoa: At home, management has several parts. First is taking medication correctly, at the right dose and time. Caregivers can help by setting reminders and checking that medicines are refilled on time. Second is monitoring. Some people need home blood sugar checks with a finger-stick device. The doctor will advise how often. This depends on the treatment plan. Keep a simple notebook, date, time, blood sugar, and any symptoms like dizziness, sweating, or unusual tiredness.
Third is food. A practical approach is half the plate vegetables, one quarter protein (fish, eggs, lean meat, tofu), and one quarter carbohydrates (rice, noodles, bread), and reduce sugary drinks and snacks. Fourth is activity. Regular walking, light strength exercises, and staying active most days helps blood sugar and reduces fall risk in older adults. Finally, foot care is essential. Check the feet daily for cuts, redness, swelling, or cracks. Wear well-fitting shoes. Seek care early for any wounds. Also keep regular checkups for eyes, kidneys, blood pressure, and cholesterol.
Reporter: Finally, what key advice would you like to share with our listeners about early detection, prevention, and long-term management of Type 2 diabetes?
Dr Trung Hoa: My key advice is, don’t wait for symptoms. If you are at risk, older age, family history, overweight, high blood pressure, history of diabetes during pregnancy, get screened. Early detection prevents future suffering. For prevention, focus on daily habits that are realistic. Reduce sugary drinks, control portion sizes, eat more vegetables and protein, and move your body regularly. Even walking after meals can help. For long-term management, aim for consistency. Take medicines as prescribed, attend follow-ups, and keep a record of blood sugar when advised. Caregivers can play a powerful role by supporting healthy meals, encouraging safe physical activity, and noticing warning signs early. Diabetes is a long journey, but with steady care, people can live a healthy, active life.
Reporter: Dr. Hoa, thank you very much for sharing your time and your valuable insights with our listeners today. Type 2 diabetes can develop quietly, but as we’ve heard, early awareness, healthy daily habits, and regular checkups can make a real difference in protecting our health. That’s all for today’s edition of Doctor at Home. Thank you for listening, and we hope the information shared today will help you and your loved ones take better care of your health. Goodbye, and see you in our next program.










